In a landmark move that could reshape public health in the United States, the American Heart Association (AHA) and the American College of Cardiology (ACC) have jointly released sweeping new guidelines aimed at curbing the nation’s escalating heart disease crisis. The updated recommendations—hailed by cardiologists as a ‘critical turning point’—prioritize early cholesterol screening, personalized risk assessments, and aggressive prevention strategies targeting Americans of all ages. With cardiovascular disease remaining the leading cause of death globally, and rising rates of obesity, diabetes, and metabolic syndrome fueling a surge in related conditions, these guidelines represent a proactive shift from reactive treatment to lifelong prevention.
- New ACC/AHA guidelines emphasize early cholesterol screening and personalized risk assessments using the PREVENT score.
- Cardiologists advocate for lifelong lifestyle interventions—diet, exercise, sleep, and smoking cessation—as first-line prevention tools.
- The guidelines target high-risk populations, including adolescents and young adults, to address cholesterol issues before they progress.
- Experts say the new approach could significantly reduce heart attacks, strokes, and heart failure by preventing plaque buildup early.
- Implementation by healthcare providers is critical to reducing the long-term burden of cardiovascular disease nationwide.
Why the New Cholesterol Guidelines Represent a Paradigm Shift in Heart Disease Prevention
Cardiovascular disease has long reigned as the deadliest threat to global health, responsible for nearly 18 million deaths annually, according to the World Health Organization. In the United States alone, heart disease claims more than 695,000 lives each year—more than all forms of cancer and chronic lower respiratory diseases combined. For decades, the standard approach to managing high cholesterol and related heart risks has focused on treating patients once symptoms appear or after a cardiac event has occurred. But the tide is turning. The newly released ACC/AHA cholesterol guidelines signal a fundamental shift toward prevention that begins in childhood and continues throughout adulthood, driven by mounting evidence that early intervention can dramatically alter long-term health outcomes.
The Role of Cholesterol in Modern Heart Disease: A Growing Crisis
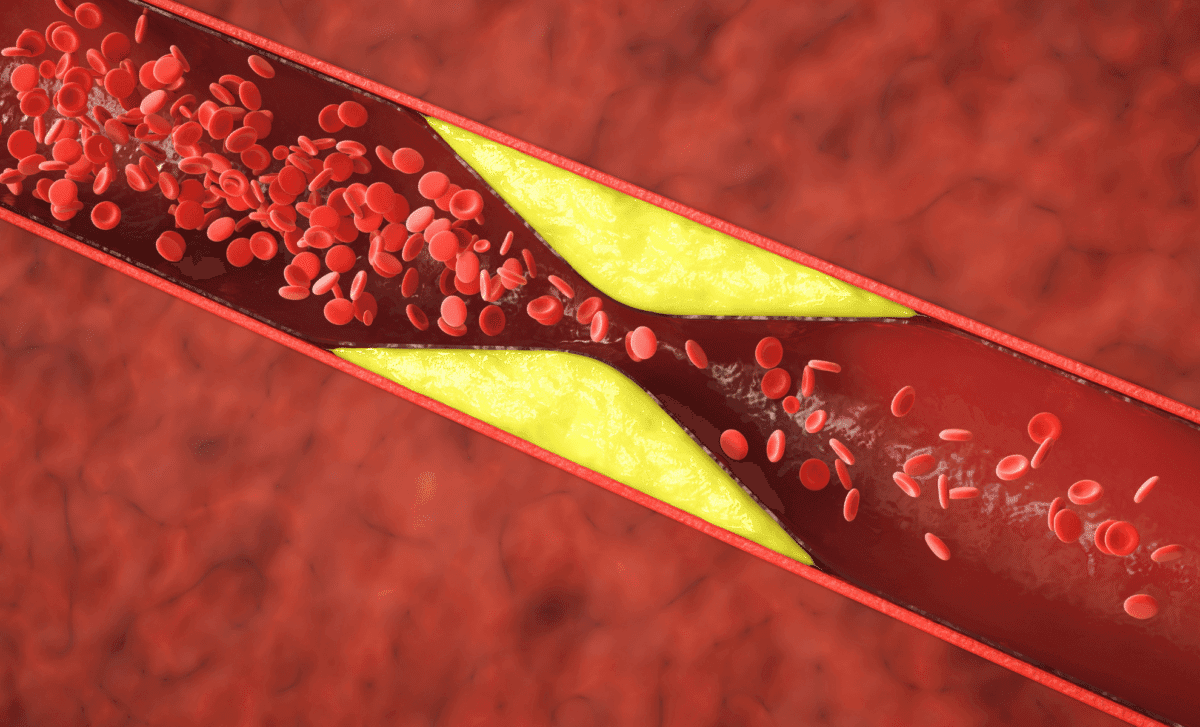
At the heart of this transformation is the recognition of cholesterol—not just as a number to be managed later in life, but as a lifelong risk factor that must be addressed proactively. Low-density lipoprotein (LDL), often dubbed ‘bad cholesterol,’ plays a central role in the buildup of atherosclerotic plaque within artery walls. Over time, this plaque narrows blood vessels, restricts blood flow, and can rupture, triggering heart attacks or strokes. While statins and other medications remain crucial tools for high-risk individuals, the new guidelines argue that medication alone is insufficient without foundational lifestyle changes and early detection.
The urgency of this shift is underscored by recent trends. The U.S. Centers for Disease Control and Prevention (CDC) reports that nearly 40% of American adults have elevated LDL cholesterol, with rates climbing among younger populations. The rise of sedentary lifestyles, ultra-processed diets high in saturated fats, and increasing rates of obesity have contributed to a sharp uptick in metabolic disorders that accelerate heart disease risk. These factors make the ACC/AHA’s focus on prevention not just timely, but essential to reversing a decades-long public health crisis.
Shifting the paradigm toward proactive prevention strategies earlier in life can meaningfully change the trajectory of cardiovascular disease and lead to better health outcomes for people decades later.
This sentiment is echoed by Seth Martin, MD, MHS, a leading cardiologist at the Johns Hopkins Ciccarone Center for the Prevention of Cardiovascular Disease and a key contributor to the new guidelines. Martin emphasizes that the updated recommendations reflect a growing consensus among experts: waiting for high cholesterol to cause damage is no longer an acceptable strategy.
New Risk Assessment Tools: How the PREVENT Score Changes the Game
One of the most innovative aspects of the updated guidelines is the endorsement of the PREVENT (Predicting Risk of Cardiovascular Disease Events) risk calculator—a sophisticated tool designed to estimate an individual’s 10- and 30-year risk of heart attack, stroke, or heart failure. Unlike traditional risk models that rely heavily on age and basic cholesterol levels, PREVENT incorporates a broader array of factors, including blood pressure, diabetes status, kidney function, and smoking history. This allows clinicians to deliver more precise, personalized risk assessments and tailor prevention plans to each patient’s unique profile.
Who Should Be Screened—and When?
The guidelines recommend cholesterol screening starting as early as age 20 for most adults, with more frequent or earlier screening advised for individuals with risk factors such as a family history of heart disease, obesity, hypertension, or type 2 diabetes. For high-risk groups—including those with a history of familial hypercholesterolemia or early-onset cardiovascular events—screening may begin in adolescence. This represents a major departure from older recommendations that often delayed testing until middle age, by which time plaque buildup may already be advanced.
Roger Blumenthal, MD, a cardiologist at Johns Hopkins and co-director of the Ciccarone Center, stresses the importance of these early interventions. ‘Lower LDL cholesterol levels are better when it comes to reducing the risk of heart attacks, strokes, and congestive heart failure,’ he explains. ‘We now know that even modest elevations in LDL in young adults can set the stage for atherosclerosis decades later.’ The guidelines encourage clinicians to aim for lower LDL targets based on individual risk, often advocating for lifestyle changes first, followed by medication when necessary.
Lower LDL cholesterol levels are better when it comes to reducing the risk of heart attacks, strokes, and congestive heart failure.
Lifestyle as Medicine: The Cornerstone of Heart Disease Prevention
While medications like statins play a vital role in managing high cholesterol, the ACC/AHA guidelines firmly position lifestyle interventions as the foundation of prevention. The updated recommendations highlight four key pillars: nutrition, physical activity, sleep hygiene, and smoking cessation. These are not merely supportive measures—they are the primary defense against the development of atherosclerotic cardiovascular disease (ASCVD).
Diet: More Than Just ‘Low-Fat’—A Focus on Whole Foods and Plant-Based Patterns
The guidelines move beyond simplistic ‘low-fat’ advice and instead promote dietary patterns rich in fruits, vegetables, whole grains, legumes, nuts, seeds, and lean proteins—particularly plant-based sources. The Mediterranean diet and the DASH (Dietary Approaches to Stop Hypertension) diet are specifically cited as models that can reduce LDL cholesterol by 10–15% when followed consistently. Reducing intake of saturated fats (found in red meat and full-fat dairy), trans fats (found in processed foods), and added sugars is strongly emphasized. The guidelines also recommend increasing soluble fiber intake, which binds to cholesterol in the digestive tract and helps remove it from the body.
Exercise: Moving from Sedentary to Active Lifestyles
Regular physical activity is another cornerstone of the new prevention strategy. The guidelines recommend at least 150 minutes of moderate-intensity aerobic exercise (such as brisk walking or cycling) per week, or 75 minutes of vigorous activity (like running or swimming), supplemented by muscle-strengthening exercises on two or more days per week. Even modest increases in activity—such as walking 30 minutes daily—can lower LDL cholesterol and improve overall cardiovascular health. For individuals with limited mobility or chronic conditions, tailored exercise programs are encouraged under medical supervision.
Sleep and Stress: The Overlooked Risk Factors
Emerging research has linked poor sleep quality and chronic stress to increased inflammation and higher cholesterol levels. The guidelines now include recommendations for 7–9 hours of quality sleep per night and stress-reduction techniques such as mindfulness, meditation, or yoga. Sleep apnea, a condition that disrupts breathing during sleep and is associated with hypertension and metabolic dysfunction, is also flagged as a high-risk factor that warrants screening and treatment.
Preventing Heart Disease Before Adulthood: A Focus on Youth
Perhaps the most groundbreaking aspect of the new guidelines is their emphasis on prevention beginning in childhood and adolescence. High cholesterol is no longer seen as an adult-only concern. In fact, atherosclerotic changes can begin in the arteries of young individuals, particularly those with genetic predispositions or poor lifestyle habits. The ACC/AHA now recommend cholesterol screening for children and adolescents with risk factors such as obesity, a family history of early heart disease, or parental history of high cholesterol or diabetes.
Taking action early in life is critical because high cholesterol begins to impact your heart disease risk even in adolescence.
Pamela Morris, MD, a cardiologist at the Medical University of South Carolina and co-chair of the guideline writing committee, highlights the urgency of this approach. ‘We have an opportunity to intervene when lifestyles are forming, habits are being set, and the body is still resilient,’ she says. ‘By teaching young people the value of heart-healthy eating, regular exercise, and avoiding tobacco, we can prevent many cardiovascular issues from ever developing.’ School-based programs, family counseling, and community initiatives are encouraged to support these efforts.
From Guidelines to Action: How Clinicians and Patients Can Implement Change
The success of these new guidelines hinges on their adoption by healthcare providers and engagement from patients. Clinicians are urged to integrate PREVENT risk scores into electronic health records, screen patients proactively, and prioritize shared decision-making in treatment plans. For patients, the message is clear: prevention is not a one-time effort but a lifelong commitment. Regular follow-ups, self-monitoring of blood pressure and cholesterol, and adherence to prescribed interventions are essential.
Overcoming Barriers to Prevention
Despite the promise of these guidelines, significant challenges remain. Cost barriers, lack of access to primary care, and disparities in healthcare delivery—particularly in rural and underserved communities—can hinder early screening and intervention. The guidelines acknowledge these obstacles and call for policy changes, expanded insurance coverage for preventive services, and public health campaigns to raise awareness. Additionally, misinformation about cholesterol and statins persists, leading some patients to avoid necessary medications out of fear or misunderstanding.
Blumenthal stresses the need for education. ‘We must do a better job communicating the science behind cholesterol management and the proven benefits of early action,’ he says. ‘This is not about scare tactics—it’s about empowering people with knowledge and support to take control of their heart health.’
We also know that bringing elevated lipids and blood pressure down in young adults supports optimal heart and vascular health throughout a person’s life.
The Long-Term Vision: A Healthier Future Through Prevention
The ACC/AHA guidelines are more than a clinical update—they represent a cultural shift in how society views heart disease. By prioritizing prevention from cradle to grave, the medical community aims to reduce the incidence of heart attacks, strokes, and heart failure not through heroic interventions after the fact, but through sustained, proactive care. If successfully implemented, these guidelines could reduce the national burden of cardiovascular disease, lower healthcare costs, and improve quality of life for millions of Americans.
Morris underscores this vision: ‘Implementation of this important new guideline by clinicians will be critical to reduce the burden of cardiovascular disease in the future.’ With heart disease affecting nearly half of all American adults and costing the U.S. healthcare system over $200 billion annually, the stakes could not be higher. The new guidelines offer a roadmap not just for doctors, but for families, schools, workplaces, and policymakers to come together and build a heart-healthier nation.
What’s Next? The Road Ahead for Heart Health in America
The release of these guidelines marks the beginning, not the end, of a broader movement. The ACC and AHA have committed to updating their recommendations regularly as new evidence emerges, including data on emerging therapies like PCSK9 inhibitors and gene-editing technologies for familial hypercholesterolemia. Public health leaders are also calling for stronger collaboration between medical societies, insurers, employers, and community organizations to create environments that support healthy choices—from tobacco-free campuses to walkable cities and affordable access to fresh foods.
Frequently Asked Questions
Frequently Asked Questions
- What are the new ACC/AHA cholesterol guidelines focused on?
- The updated guidelines prioritize early cholesterol screening using the PREVENT risk score, personalized risk assessments, and lifelong lifestyle interventions including diet, exercise, sleep, and smoking cessation as the cornerstone of prevention.
- At what age should adults start getting cholesterol screenings?
- The guidelines recommend cholesterol screening starting at age 20 for most adults, with earlier screening advised for high-risk individuals such as those with a family history of heart disease, obesity, or diabetes.
- Can lifestyle changes really lower cholesterol enough to prevent heart disease?
- Yes. Following a Mediterranean or DASH diet, engaging in regular physical activity, improving sleep, and avoiding smoking can reduce LDL cholesterol by 10–15% and significantly lower long-term heart disease risk.